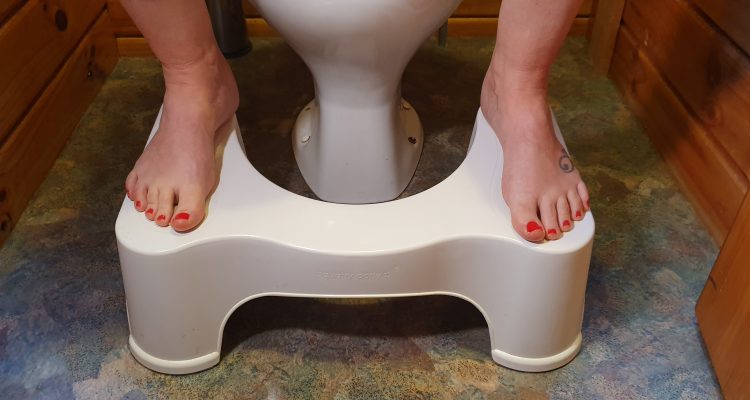
Defecation dynamics
The stools can come out easier if you are in the right position to allow the muscles to relax properly. Our friends over at Squatty Potty, have done a swell job at explaining how this works! We have toilet stools available for purchase at the clinic to help you poop like a unicorn. Whack your feet up on one so your knees are higher than your hips, to really feel the motion of the ocean when releasing the hamsters. Never strain but take your time, leaning forward and with your lower tummy completely relaxed and happy to ‘nudge’ the nugget.
We may need to work more intensively to teach you how to relax the muscles at the right time, as well as retrain what it feels like to have a normal sized poo in the rectum ready to pass, and responding to that sensation. We advise on the best techniques for you to empty your bowel fully and regularly and combined with manipulation of the stools to be more soft, formed and easy to pass… this is a gateway towards the best poo of your life!